Small Intestine
The small intestine (or small bowel) is the part of the gastrointestinal tract following the stomach and followed by the large intestine, and is where much of the digestion and absorption of food takes place. In invertebrates such as worms, the terms "gastrointestinal tract" and "large intestine" are often used to describe the entire intestine. This article is primarily about the human gut, though the information about its processes is directly applicable to most placental mammals. The primary function of the small intestine is the absorption of nutrients and minerals found in food.
The average length of the small intestine in an adult human male is 6.9 m (22 feet 6 inches), and in the adult female 7.1 m (23 feet 4 inches). It can vary greatly, from as short as 4.6 m (15 feet) to as long as 9.8 m (32 feet)
The average length of the small intestine in an adult human male is 6.9 m (22 feet 6 inches), and in the adult female 7.1 m (23 feet 4 inches). It can vary greatly, from as short as 4.6 m (15 feet) to as long as 9.8 m (32 feet)
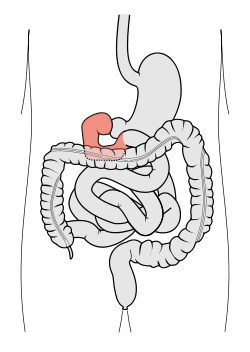
The Duodenum; colored in Red
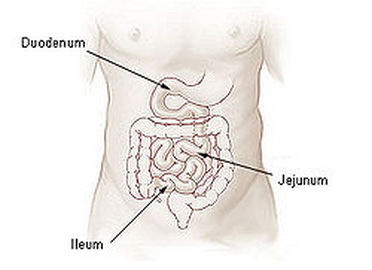
The First Segment - Duodenum
The duodenum is the first section of the small intestine in most higher vertebrates, including mammals, reptiles, and birds. In fish, the divisions of the small intestine are not as clear, and the terms anterior intestine or proximal intestine may be used instead of duodenum. In mammals the duodenum may be the principal site for iron absorption.
The duodenum precedes the jejunum and ileum and is the shortest part of the small intestine, where most chemical digestion takes place. The name duodenum is from the Latin duodenum digitorum, or twelve fingers' breadths.
In humans, the duodenum is a hollow jointed tube about 10–15 inches (25–38 centimetres) long connecting the stomach to the jejunum.
The duodenum precedes the jejunum and ileum and is the shortest part of the small intestine, where most chemical digestion takes place. The name duodenum is from the Latin duodenum digitorum, or twelve fingers' breadths.
In humans, the duodenum is a hollow jointed tube about 10–15 inches (25–38 centimetres) long connecting the stomach to the jejunum.
The Second Segment - Jejunum
The jejunum is the middle section of the small intestine in most higher vertebrates, including mammals, reptiles, and birds. In fish, the divisions of the small intestine are not as clear and the terms middle intestine or mid-gut may be used instead of jejunum.
The jejunum lies between the duodenum and the ileum. The change from the duodenum to the jejunum is usually defined as the Duodenojejunal flexure and is attached, and thus "hung up", to the ventricle (see stomach) by the ligament of Treitz. In adult humans, the small intestine is usually between 5.5 and 6m long, 2.5m of which is the jejunum.
The pH in the jejunum is usually between 7 and 9 (neutral or slightly alkaline). If the jejunum is impacted by blunt force the emesis reflex will be initiated.
The jejunum and the ileum are suspended by mesentery which gives the bowel great mobility within the abdomen. It also contains circular and longitudinal smooth muscle which helps to move food along by a process known as peristalsis.
The jejunum lies between the duodenum and the ileum. The change from the duodenum to the jejunum is usually defined as the Duodenojejunal flexure and is attached, and thus "hung up", to the ventricle (see stomach) by the ligament of Treitz. In adult humans, the small intestine is usually between 5.5 and 6m long, 2.5m of which is the jejunum.
The pH in the jejunum is usually between 7 and 9 (neutral or slightly alkaline). If the jejunum is impacted by blunt force the emesis reflex will be initiated.
The jejunum and the ileum are suspended by mesentery which gives the bowel great mobility within the abdomen. It also contains circular and longitudinal smooth muscle which helps to move food along by a process known as peristalsis.
The ileum /ˈɪliːəm/ is the final section of the small intestine in most higher vertebrates, including mammals, reptiles, and birds. In fish, the divisions of the small intestine are not as clear and the terms posterior intestine or distal intestine may be used instead of ileum.
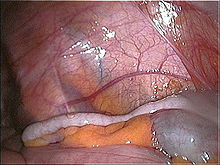
The ileum follows the duodenum and jejunum and is separated from the cecum by the ileocecal valve (ICV). In humans, the ileum is about 2–4 m long, and the pH is usually between 7 and 8 (neutral or slightly alkaline).
The function of the ileum is mainly to absorb vitamin B12 and bile salts and whatever products of digestion that were not absorbed by the jejunum. The wall itself is made up of folds, each of which has many tiny finger-like projections known as villi on its surface. In turn, the epithelial cells that line these villi possess even larger numbers of microvilli. Therefore the ileum has an extremely large surface area both for the adsorption (attachment) of enzyme molecules and for the absorption of products of digestion. The DNES (diffuse neuroendocrine system) cells of the ileum secrete various hormones (gastrin, secretin, cholecystokinin) into the blood. Cells in the lining of the ileum secrete the protease and carbohydrase enzymes responsible for the final stages of protein and carbohydrate digestion into the lumen of the intestine. These enzymes are present in the cytoplasm of the epithelial cells.
The villi contain large numbers of capillaries that take the amino acids and glucose produced by digestion to the hepatic portal vein and the liver. Lacteals are small lymph vessels, and are present in villi. They absorb fatty acid and glycerol, the products of fat digestion. Layers of circular and longitudinal smooth muscle enable the digested food to be pushed along the ileum by waves of muscle contractions called peristalsis. The undigested food (waste and water) are sent to the colon.
The ileum follows the duodenum and jejunum and is separated from the cecum by the ileocecal valve (ICV). In humans, the ileum is about 2–4 m long, and the pH is usually between 7 and 8 (neutral or slightly alkaline).
The function of the ileum is mainly to absorb vitamin B12 and bile salts and whatever products of digestion that were not absorbed by the jejunum. The wall itself is made up of folds, each of which has many tiny finger-like projections known as villi on its surface. In turn, the epithelial cells that line these villi possess even larger numbers of microvilli. Therefore the ileum has an extremely large surface area both for the adsorption (attachment) of enzyme molecules and for the absorption of products of digestion. The DNES (diffuse neuroendocrine system) cells of the ileum secrete various hormones (gastrin, secretin, cholecystokinin) into the blood. Cells in the lining of the ileum secrete the protease and carbohydrase enzymes responsible for the final stages of protein and carbohydrate digestion into the lumen of the intestine. These enzymes are present in the cytoplasm of the epithelial cells.
The villi contain large numbers of capillaries that take the amino acids and glucose produced by digestion to the hepatic portal vein and the liver. Lacteals are small lymph vessels, and are present in villi. They absorb fatty acid and glycerol, the products of fat digestion. Layers of circular and longitudinal smooth muscle enable the digested food to be pushed along the ileum by waves of muscle contractions called peristalsis. The undigested food (waste and water) are sent to the colon.
Function of the Small Intestines
Digestion - The small intestine is where most chemical digestion takes place. Most of the digestive enzymes that act in the small intestine are secreted by the pancreas and enter the small intestine via the pancreatic duct. Enzymes enter the small intestine in response to the hormone cholecystokinin, which is produced in the small intestine in response to the presence of nutrients. The hormone secretin also causes bicarbonate to be released into the small intestine from the pancreas in order to neutralize the potentially harmful acid coming from the stomach.
The three major classes of nutrients that undergo digestion are proteins, lipids (fats) and carbohydrates:
A.) Proteins are degraded into small peptides and amino acids before absorption. Chemical breakdown begins in the stomach and continues in the large intestine. Proteolytic enzymes, including trypsin and chymotrypsin, are secreted by the pancreas and cleave proteins into smaller peptides. Carboxypeptidase, which is a pancreatic brush border enzyme, splits one amino acid at a time. Aminopeptidase and dipeptidase free the end amino acid products.
B.) Lipids (fats) are degraded into fatty acids and glycerol. Pancreatic lipase breaks down triglycerides into free fatty acids and monoglycerides. Pancreatic lipase works with the help of the salts from the bile secreted by the liver and the gall bladder. Bile salts attach to triglycerides to help emulsify them, which aids access by pancreatic lipase. This occurs because the lipase is water-soluble but the fatty triglycerides are hydrophobic and tend to orient towards each other and away from the watery intestinal surroundings. The bile salts are the "main man" that holds the triglycerides in the watery surroundings until the lipase can break them into the smaller components that are able to enter the villi for absorption.
C.) Some carbohydrates are degraded into simple sugars, or monosaccharides (e.g., glucose). Pancreatic amylase breaks down some carbohydrates (notably starch) into oligosaccharides. Other carbohydrates pass undigested into the large intestine and further handling by intestinal bacteria. Brush border enzymes take over from there. The most important brush border enzymes are dextrinase and glucoamylase which further break down oligosaccharides. Other brush border enzymes are maltase, sucrase and lactase. Lactase is absent in most adult humans and for them lactose, like most poly-saccharides, are not digested in the small intestine. Some carbohydrates, such as cellulose, are not digested at all, despite being made of multiple glucose units. This is because the cellulose is made out of beta-glucose, making the inter-monosaccharidal bindings different from the ones present in starch, which consists of alpha-glucose. Humans lack the enzyme for splitting the beta-glucose-bonds, something reserved for herbivores and bacteria from the large intestine.
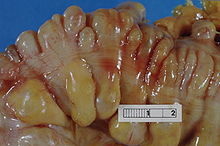
Absorption - Digested food is now able to pass into the blood vessels in the wall of the intestine through the process of diffusion. The small intestine is the site where most of the nutrients from ingested food are absorbed. The inner wall, or mucosa, of the small intestine is lined with simple columnar epithelial tissue. Structurally, the mucosa is covered in wrinkles or folds called plicae circulares, which are considered permanent features in the wall of the organ. They are distinct from rugae which are considered non-permanent or temporary allowing for distention and contraction. From the plicae circulares project microscopic finger-like pieces of tissue called villi (Latin for "shaggy hair"). The individual epithelial cells also have finger-like projections known as microvilli. The function of the plicae circulares, the villi and the microvilli is to increase the amount of surface area available for the absorption of nutrients.
Each villus has a network of capillaries and fine lymphatic vessels called lacteals close to its surface. The epithelial cells of the villi transport nutrients from the lumen of the intestine into these capillaries (amino acids and carbohydrates) and lacteals (lipids). The absorbed substances are transported via the blood vessels to different organs of the body where they are used to build complex substances such as the proteins required by our body. The food that remains undigested and unabsorbed passes into the large intestine.
The three major classes of nutrients that undergo digestion are proteins, lipids (fats) and carbohydrates:
A.) Proteins are degraded into small peptides and amino acids before absorption. Chemical breakdown begins in the stomach and continues in the large intestine. Proteolytic enzymes, including trypsin and chymotrypsin, are secreted by the pancreas and cleave proteins into smaller peptides. Carboxypeptidase, which is a pancreatic brush border enzyme, splits one amino acid at a time. Aminopeptidase and dipeptidase free the end amino acid products.
B.) Lipids (fats) are degraded into fatty acids and glycerol. Pancreatic lipase breaks down triglycerides into free fatty acids and monoglycerides. Pancreatic lipase works with the help of the salts from the bile secreted by the liver and the gall bladder. Bile salts attach to triglycerides to help emulsify them, which aids access by pancreatic lipase. This occurs because the lipase is water-soluble but the fatty triglycerides are hydrophobic and tend to orient towards each other and away from the watery intestinal surroundings. The bile salts are the "main man" that holds the triglycerides in the watery surroundings until the lipase can break them into the smaller components that are able to enter the villi for absorption.
C.) Some carbohydrates are degraded into simple sugars, or monosaccharides (e.g., glucose). Pancreatic amylase breaks down some carbohydrates (notably starch) into oligosaccharides. Other carbohydrates pass undigested into the large intestine and further handling by intestinal bacteria. Brush border enzymes take over from there. The most important brush border enzymes are dextrinase and glucoamylase which further break down oligosaccharides. Other brush border enzymes are maltase, sucrase and lactase. Lactase is absent in most adult humans and for them lactose, like most poly-saccharides, are not digested in the small intestine. Some carbohydrates, such as cellulose, are not digested at all, despite being made of multiple glucose units. This is because the cellulose is made out of beta-glucose, making the inter-monosaccharidal bindings different from the ones present in starch, which consists of alpha-glucose. Humans lack the enzyme for splitting the beta-glucose-bonds, something reserved for herbivores and bacteria from the large intestine.
Absorption - Digested food is now able to pass into the blood vessels in the wall of the intestine through the process of diffusion. The small intestine is the site where most of the nutrients from ingested food are absorbed. The inner wall, or mucosa, of the small intestine is lined with simple columnar epithelial tissue. Structurally, the mucosa is covered in wrinkles or folds called plicae circulares, which are considered permanent features in the wall of the organ. They are distinct from rugae which are considered non-permanent or temporary allowing for distention and contraction. From the plicae circulares project microscopic finger-like pieces of tissue called villi (Latin for "shaggy hair"). The individual epithelial cells also have finger-like projections known as microvilli. The function of the plicae circulares, the villi and the microvilli is to increase the amount of surface area available for the absorption of nutrients.
Each villus has a network of capillaries and fine lymphatic vessels called lacteals close to its surface. The epithelial cells of the villi transport nutrients from the lumen of the intestine into these capillaries (amino acids and carbohydrates) and lacteals (lipids). The absorbed substances are transported via the blood vessels to different organs of the body where they are used to build complex substances such as the proteins required by our body. The food that remains undigested and unabsorbed passes into the large intestine.
Large Intestine
The large intestine (or large bowel) is the third-to-last part of the digestive system in vertebrate animals. Its function is to absorb water from the remaining indigestible food matter, and then to pass useless waste material from the body.
The large intestine consists of the cecum and colon. It starts in the right iliac region of the pelvis, just at or below the right waist, where it is joined to the bottom end of the small intestine. From here it continues up the abdomen, then across the width of the abdominal cavity, and then it turns down, continuing to its endpoint at the anus.
The large intestine is about 4.9 feet (1.5 m) long, which is about one-fifth of the whole length of the intestinal canal.
The large intestine consists of the cecum and colon. It starts in the right iliac region of the pelvis, just at or below the right waist, where it is joined to the bottom end of the small intestine. From here it continues up the abdomen, then across the width of the abdominal cavity, and then it turns down, continuing to its endpoint at the anus.
The large intestine is about 4.9 feet (1.5 m) long, which is about one-fifth of the whole length of the intestinal canal.
Functions of the Large Intestines
The large intestine takes about 16 hours to finish up the remaining processes of the digestive system. Food is no longer broken down at this stage of digestion. The colon absorbs vitamins which are created by the colonic bacteria - such as vitamin K (especially important as the daily ingestion of vitamin K is not normally enough to maintain adequate blood coagulation), vitamin B12, thiamine and riboflavin. It also compacts faeces, and stores fecal matter in the rectum until it can be discharged via the anus in defecation.
The large intestine differs in physical form from the small intestine in being much wider and in showing the longitudinal layer of the muscularis have been reduced to 3 strap-like structures known as the taeniae coli. The wall of the large intestine is lined with simple columnar epithelium. Instead of having the evaginations of the small intestine (villi), the large intestine has invaginations (the intestinal glands). While both the small intestine and the large intestine have goblet cells, they are abundant in the large intestine.
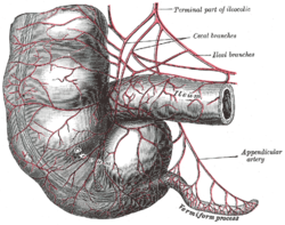
The appendix is attached to its inferior surface of the cecum. It contains the least of lymphoid tissue. It is a part of mucosa-associated lymphoid tissue, which gives the appendix an important role in immunity. Appendicitis is the result of a blockage that traps infectious material in the lumen. The appendix can be removed with no apparent damage or consequence to the patient. The large intestine extends from the ileocecal junction to the anus and is about 4.9 ft long. On the surface, bands of longitudinal muscle fibers called taeniae coli, each about 1/5 in wide, can be identified.
There are three bands, and they start at the base of the appendix and extend from the cecum to the rectum. Along the sides of the taeniae, tags of peritoneum filled with fat, called epiploic appendages (or appendices epiploicae) are found. The sacculations, called haustra, are characteristic features of the large intestine, and distinguish it from the small intestine.
The large intestine differs in physical form from the small intestine in being much wider and in showing the longitudinal layer of the muscularis have been reduced to 3 strap-like structures known as the taeniae coli. The wall of the large intestine is lined with simple columnar epithelium. Instead of having the evaginations of the small intestine (villi), the large intestine has invaginations (the intestinal glands). While both the small intestine and the large intestine have goblet cells, they are abundant in the large intestine.
The appendix is attached to its inferior surface of the cecum. It contains the least of lymphoid tissue. It is a part of mucosa-associated lymphoid tissue, which gives the appendix an important role in immunity. Appendicitis is the result of a blockage that traps infectious material in the lumen. The appendix can be removed with no apparent damage or consequence to the patient. The large intestine extends from the ileocecal junction to the anus and is about 4.9 ft long. On the surface, bands of longitudinal muscle fibers called taeniae coli, each about 1/5 in wide, can be identified.
There are three bands, and they start at the base of the appendix and extend from the cecum to the rectum. Along the sides of the taeniae, tags of peritoneum filled with fat, called epiploic appendages (or appendices epiploicae) are found. The sacculations, called haustra, are characteristic features of the large intestine, and distinguish it from the small intestine.
The Cecum (Left)
Taeniae Coli muscles running along the Sigmoid Colon
The Haustra; which are bulging sac-like pouches; giving the Colon's segmented look
The Epiploic Appendages; which are more known as Appendix
Parts of the Large Intestine
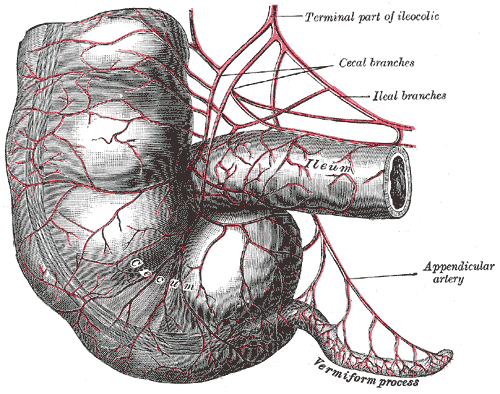
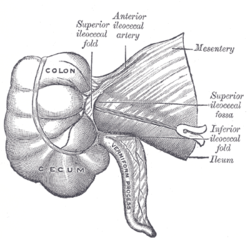
Cecum - Is a pouch, usually peritoneal, that is considered to be the beginning of the large intestine. It receives fecal material from the ileum, and connects to the ascending colon of the large intestine. It is separated from the ileum by the ileocecal valve (ICV) or Bauhin's valve. It is also separated from the colon by the cecocolic junction (A gap).
Taeniae Coli - These are three separate longitudinal ribbons of smooth muscle on the outside of the ascending, transverse, descending and sigmoid colons. They are visible, and can be seen just below the serosa or fibrosa. They are the Mesocolic, Free and Omental Coli. The teniae coli contract lengthwise to produce the haustra, the bulges in the colon. The bands converge at the root of the vermiform appendix and the rectum.
These bands correspond to the outer layer of the muscularis externa, in other portions of the digestive tract.
Haustra - The haustra (singular haustrum) of the colon are the small pouches caused by sacculation, which give the colon its segmented appearance. The taenia coli runs the length of the large intestine. Because the taenia coli is shorter than the intestine, the colon becomes sacculated between the taenia, forming the haustra.
Epiploic Appendages - are small pouches of the peritoneum filled with fat and situated along the colon and upper part of the rectum.They are chiefly appended to the transverse and sigmoid parts of the colon, however, their function is unknown.
The appendages can become inflamed, a benign but painful process known as epiploic appendagitis which can mimic acute appendicitis and other conditions.
Taeniae Coli - These are three separate longitudinal ribbons of smooth muscle on the outside of the ascending, transverse, descending and sigmoid colons. They are visible, and can be seen just below the serosa or fibrosa. They are the Mesocolic, Free and Omental Coli. The teniae coli contract lengthwise to produce the haustra, the bulges in the colon. The bands converge at the root of the vermiform appendix and the rectum.
These bands correspond to the outer layer of the muscularis externa, in other portions of the digestive tract.
Haustra - The haustra (singular haustrum) of the colon are the small pouches caused by sacculation, which give the colon its segmented appearance. The taenia coli runs the length of the large intestine. Because the taenia coli is shorter than the intestine, the colon becomes sacculated between the taenia, forming the haustra.
Epiploic Appendages - are small pouches of the peritoneum filled with fat and situated along the colon and upper part of the rectum.They are chiefly appended to the transverse and sigmoid parts of the colon, however, their function is unknown.
The appendages can become inflamed, a benign but painful process known as epiploic appendagitis which can mimic acute appendicitis and other conditions.
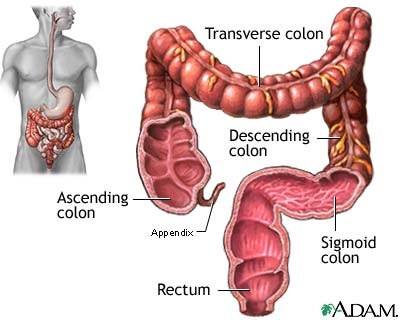
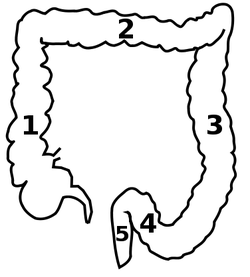
Schematical Image of the Large Intestine (1) Ascending Colon, (2) Transverse Colon, (3) Descending Colon, (4) Sigmoid Colon;
and lastly the Rectum; which leads to the Anal Canal
and lastly the Rectum; which leads to the Anal Canal
Ascending Colon - The ascending colon is smaller in caliber than the cecum.It passes upward, from its commencement at the cecum, opposite the colic valve, to the under surface of the right lobe of the liver, on the right of the gall-bladder, where it is lodged in a shallow depression, the colic impression; here it bends abruptly forward and to the left, forming the right colic flexure (hepatic).
Transverse Colon - The longest and most movable part of the colon, passes with a downward convexity from the right hypochondrium region across the abdomen, opposite the confines of the epigastric and umbilical zones, into the left hypochondrium region, where it curves sharply on itself beneath the lower end of the spleen, forming the splenic or left colic flexure. The right colic flexure is adjacent to the liver.
Descending Colon - Part of the large intestine that passes downward along the lateral border of the left kidney
Sigmoid Colon - It is a part of the large intestine that is closest to the rectum and anus. It forms a loop that averages about 40 cm in length, and normally lies within the pelvis.
Transverse Colon - The longest and most movable part of the colon, passes with a downward convexity from the right hypochondrium region across the abdomen, opposite the confines of the epigastric and umbilical zones, into the left hypochondrium region, where it curves sharply on itself beneath the lower end of the spleen, forming the splenic or left colic flexure. The right colic flexure is adjacent to the liver.
Descending Colon - Part of the large intestine that passes downward along the lateral border of the left kidney
Sigmoid Colon - It is a part of the large intestine that is closest to the rectum and anus. It forms a loop that averages about 40 cm in length, and normally lies within the pelvis.